Claimable Blog
Learn about appeals, denials, and stay up to date on what is happening in the world of healthcare.

Your doctor prescribed Ubrelvy because it's the right acute treatment for your migraines — and in many cases, because triptans aren't safe or effective for you. Your insurer disagreed. But a denial letter isn't the final word, and you have more power to challenge it than you probably realize.
Ubrelvy (ubrogepant) was the first oral calcitonin gene-related peptide (CGRP) medication FDA-approved specifically for treating migraine attacks. It works through an entirely different mechanism than triptans — blocking the CGRP protein involved in migraine pain, nausea, and sensitivity to light and sound, rather than constricting blood vessels. That distinction matters clinically, and it matters enormously when it comes to insurance coverage, because the very reason your doctor chose Ubrelvy is often the reason your insurer tries to deny it.
Here's what AbbVie's own access data shows: 56% of commercially insured patients are unrestricted or need only minimal prior therapy to access Ubrelvy. That means nearly half face significant coverage hurdles — prior authorization requirements, step therapy demands, or outright denials. If you're reading this, you're likely in that group.
The good news: denials can be overturned. Fewer than 1% of denied claims are ever appealed, and insurance companies bank on that silence. But when patients appeal with the right evidence and strategy, the results are dramatically different. At Claimable, over 80% of our appeals succeed in established conditions.
This guide breaks down exactly why Ubrelvy gets denied, how to identify your specific situation, and what a winning appeal looks like — including the clinical arguments, legal protections, and documentation strategies that actually move the needle.
Why Insurance Companies Deny Ubrelvy
The single most important thing to do before anything else: understand the specific reason your insurer denied coverage. The denial reason shapes your entire appeal strategy. Getting it wrong means building a case that doesn't address the actual barrier.
The Triptan Paradox: Why Ubrelvy Denials Are Often Medically Absurd
Here's the central irony of most Ubrelvy denials: your doctor likely prescribed Ubrelvy because triptans don't work for you, cause intolerable side effects, or are medically unsafe given your health history. And your insurer's most likely response is to demand that you try more triptans first.
This isn't a minor bureaucratic inconvenience. Research published in the Journal of Primary Care & Community Health found that more than 20% of commercially insured migraine patients have a cardiovascular condition that specifically contraindicates triptan use — conditions like coronary artery disease, peripheral vascular disease, uncontrolled hypertension, or history of stroke. An additional 25% have multiple cardiovascular risk factors that carry formal warnings and precautions against triptan use. That's nearly half of all migraine patients for whom triptans are either unsafe or require serious caution.
Triptans work by constricting blood vessels. That vasoconstriction is the source of both their efficacy and their risk. Ubrelvy doesn't constrict blood vessels at all — it targets the CGRP receptor, addressing migraine pain through an entirely different pathway. For patients with cardiovascular concerns, this isn't a preference. It's a medical necessity.
When an insurer requires you to try and fail triptans before approving Ubrelvy, and your medical history includes cardiovascular contraindications, they're effectively asking you to take medications your own doctor has determined could put your health at risk. That's a powerful foundation for an appeal.
Even for patients without cardiovascular issues, there are legitimate clinical reasons triptans may not be appropriate: intolerable side effects (chest tightness, tingling, fatigue), medication interactions, or simply inadequate relief. Roughly one-third of migraine patients don't respond well to triptans or can't tolerate them. Ubrelvy was developed precisely for this population.
The Most Common Ubrelvy Denial Types
Every denial letter uses insurer language designed to sound definitive. Understanding what each denial type actually means — and where the insurer's reasoning is weakest — is how you build a targeted appeal.
Step Therapy Required
This is the most frequent reason Ubrelvy is denied. Major insurers including Anthem Blue Cross, Aetna, Blue Shield, and UnitedHealthcare all typically require prior authorization for Ubrelvy, and most mandate documented failure of at least two triptans before they'll approve a gepant for acute migraine treatment. Some plans require even more — failure of triptans plus NSAIDs, or failure of specific named triptans (sumatriptan, rizatriptan) rather than the class broadly. Specific step therapy requirements vary by plan and even by state, so check your denial letter for the exact criteria your insurer applied.
The critical detail most patients miss: "failure" has a broad medical definition that works in your favor. You don't have to prove a triptan was completely ineffective. Side effects count. Contraindications count. Medical reasons a drug is inappropriate for you — cardiovascular disease, medication interactions, hemiplegic migraine — all qualify as failure. If your doctor determined triptans aren't safe for you, that is a documented failure, even if you never took a single dose.
The American Headache Society's 2021 consensus statement specifically recommends gepants like Ubrelvy for patients who have failed, cannot tolerate, or have contraindications to triptans. And the AHS's 2024 position statement goes further, establishing CGRP-targeting therapies as a first-line option for migraine treatment without requiring prior failure of older drug classes. When your insurer demands triptan trials that your doctor has already ruled out, they're contradicting the leading medical society in headache medicine.
Not Medically Necessary
This denial usually means the paperwork was too thin — not that someone carefully reviewed your history and concluded Ubrelvy isn't appropriate. The most common gaps: not specifying migraine frequency and severity, not listing prior treatments tried and why they failed, not documenting impact on daily functioning, or not explaining why Ubrelvy specifically is the right choice over other acute options.
For Ubrelvy, your prescriber's documentation should make clear why a non-vasoconstrictive acute treatment is needed. If you have cardiovascular risk factors, those need to be spelled out explicitly. If you tried triptans and experienced side effects, those side effects need to be named and described, not just referenced in passing.
Quantity Limit Exceeded
Insurer quantity limits for Ubrelvy vary more than you might expect. Some plans cap coverage at 8 tablets per month, others at 10, and some allow up to 16 (which is what AbbVie packages as a standard prescription). Ubrelvy's prescribing information notes that treating more than 8 migraines in a 30-day period hasn't been studied for safety — but that's 8 migraines, not 8 tablets. Since patients can take a second dose 2 hours after the first if needed, someone treating 4–5 migraines per month with an optional second dose may legitimately need more than 8 tablets.
If your insurer denied based on quantity, your prescriber should submit documentation confirming the clinical rationale for the prescribed amount — including migraine frequency, whether a second dose is typically needed, and why the quantity is medically appropriate.
Not on Formulary / Non-Preferred Brand
Some plans position Nurtec as their preferred CGRP medication over Ubrelvy, since Nurtec carries both acute and preventive indications. Others prefer neither and want you on triptans entirely. If your plan prefers a different medication, the appeal needs to explain why Ubrelvy specifically is the right choice for your situation.
Strong arguments for a formulary exception include: you've already tried and failed the preferred alternative, the preferred drug is contraindicated for you, or there are specific clinical reasons Ubrelvy is more appropriate. If your prescriber chose Ubrelvy because you need acute-only treatment and the other options haven't worked or aren't suitable, that rationale needs to be documented clearly.
Dose-Level Denial (50mg vs. 100mg)
Some insurers will approve Ubrelvy at the 50mg dose but deny the 100mg. Both doses showed similar rates of pain freedom in the ACHIEVE trials — 21% at 2 hours for both 50mg and 100mg — but the 100mg dose was the one studied in the landmark PRODROME trial and is often the dose prescribed for patients with more severe or harder-to-treat migraines. Dose modifications are also required for patients on certain medications, which can affect which strength is clinically appropriate.
If your insurer denied the 100mg dose, your prescriber should provide a clinical rationale: why the higher dose is needed, whether the 50mg was tried and found insufficient, or whether dose adjustments related to other medications require the 100mg formulation.
Duplicate CGRP Therapy Denial
If you're already taking an injectable CGRP medication for prevention — Aimovig (erenumab), Ajovy (fremanezumab), Emgality (galcanezumab), or Vyepti (eptinezumab) — some insurers will deny Ubrelvy on the grounds that you can't use two CGRP-targeting drugs at the same time.
This denial is frequently wrong. Ubrelvy (an oral CGRP receptor antagonist for acute use) and injectable CGRP monoclonal antibodies (for prevention) work through different mechanisms and serve different clinical purposes. Published research in Advances in Therapy (Blumenfeld et al., 2022) specifically evaluated the safety and efficacy of ubrogepant in patients taking concomitant preventive CGRP monoclonal antibodies — and found no negative impact on either safety or efficacy. The Ubrelvy prescribing information itself notes that patients in clinical trials were able to use concomitant preventive medications.
A detailed clinical rationale from your neurologist or headache specialist explaining the different mechanisms, distinct indications, and published evidence supporting combination use is typically what's needed to overturn this type of denial.
Incorrect Diagnosis Code
Like all migraine medications, Ubrelvy coverage can hinge on whether the right ICD-10 code was submitted. Using a general headache code (like R51.9 for "headache, unspecified") instead of a specific migraine code will often trigger an automatic denial. The most common migraine diagnosis codes that support Ubrelvy coverage include: migraine without aura (G43.00, G43.01), migraine with aura (G43.10, G43.11), migraine unspecified (G43.90, G43.91), and chronic migraine (G43.709, G43.711).
If your denial seems to stem from a coding issue, this is usually the easiest fix — work with your prescriber's office to verify the correct code was submitted and resubmit if needed.
How to Appeal a Ubrelvy Denial: Step by Step
The insurance industry has conditioned patients to treat a denial as a final answer. It's not. Appeals are a legal right, and they work far more often than most people expect.
Step 1: Read Your Denial Letter Carefully
Every denial letter is legally required to include three things: the specific reason for denial, your appeal rights, and the deadline to file. Find the deadline first — it's the most time-sensitive detail. Most commercial plans give 180 days, but timelines vary by insurer. UnitedHealthcare allows just 65 days for most plan types. Medicare Advantage plans follow CMS guidelines of 60 days. Missing the deadline eliminates your right to appeal, so move quickly.
Step 2: Know That You Can File Your Own Appeal
Patient-initiated appeals are separate from (and in addition to) anything your doctor's office files. This is a distinction most people don't know about, and it matters. Patient appeals carry their own legal protections — mandated response timelines, the right to escalate to independent external review, and multiple levels of appeal. If your doctor's prior authorization was denied, that doesn't close the door for you. You have your own path.
Step 3: Confirm the Clinical Details With Your Prescriber
Before building your appeal, verify with your doctor's office: Was the correct migraine diagnosis code submitted? Were prior triptan trials (or contraindications to triptans) documented? Was the prescribed dose and quantity clearly justified? If the denial stems from a paperwork gap rather than a genuine coverage dispute, a corrected prior authorization resubmission may resolve the issue without a formal appeal.
Step 4: Get a Letter of Medical Necessity
A letter of medical necessity from your prescribing physician is the most important document in your appeal package. For Ubrelvy specifically, this letter should include your migraine diagnosis and frequency, a detailed history of prior treatments tried and outcomes (especially triptans — why they failed, caused side effects, or are contraindicated), any cardiovascular conditions or risk factors that make triptans unsafe, the specific clinical rationale for why Ubrelvy is the appropriate treatment, and the prescribed dose and quantity with medical justification.
How to ask: Be direct with your doctor. "My insurance denied Ubrelvy. Would you write a letter of medical necessity for my appeal? I can bring information on what the insurer typically requires." If your doctor's office isn't experienced with these, offering to share a template or outline can make a significant difference.
Step 5: Build Your Appeal Package
A complete appeal submission should include a cover letter summarizing your case, the letter of medical necessity from your prescriber, supporting clinical documentation (office visit notes showing migraine frequency, treatment history, cardiovascular history if relevant), and a personal statement explaining how the denial affects your health and daily life.
The three pillars of a winning appeal:
Your story — How migraines impact your daily life, your work, your relationships. How the denial has affected your ability to manage your condition. This isn't filler — it provides the human context that clinical data alone can't convey.
Clinical evidence — The ACHIEVE trial results, the AHS consensus statements, specific evidence supporting Ubrelvy for your situation. If cardiovascular contraindications to triptans are part of your case, the published research on triptan contraindication prevalence strengthens the argument that Ubrelvy isn't a luxury — it's a necessity.
Policy and legal analysis — How your situation meets coverage criteria under your specific plan, applicable state laws, and federal regulations like the ACA's protections for appeals and external review.
Step 6: Submit and Track
Follow the submission instructions in your denial letter exactly. Your insurer is required to respond within 30 days for standard appeals or 72 hours for urgent/expedited cases. Document everything: when you submitted, how (fax, mail, portal), and any confirmation numbers or reference IDs.
Step 7: Escalate If Needed
If your internal appeal is denied, you have the right to an external review by an independent third party who doesn't work for the insurer. External reviewers evaluate whether the denial was medically justified, not whether the insurer wants to pay. These reviews frequently overturn denials that make it to this stage, because the standard of review shifts from the insurer's internal criteria to objective clinical evidence.
Don't stop after the first "no." The appeals process exists because denials are often wrong. Persistence isn't just an emotional decision, it's a strategic one.
An Easier Path: Let Claimable Handle Your Ubrelvy Appeal
If the process above feels like a lot, or if you've already been through one round of denials and don't have the energy for another, Claimable can take it from here.
Here's how it works:
Answer a few questions about your Ubrelvy denial and medical history. We build your case using our database of 4+ million clinical studies, insurer policies, and legal standards. We create a fully customized appeal with your personal story, clinical evidence, and policy analysis. We submit it for you — faxed and mailed directly to your insurer. We guide you through escalation if needed.
Over 80% of Claimable appeals succeed, with most resolved in 10 days or less.
"When my insurance company denied my claim to continue with my medicine, I felt defeated at first… Then I found Claimable. In the end I ended up winning my claim and I couldn't have done it without Claimable. I highly recommend them." – April A.
Appealing with Claimable costs $39.95. No success fees, no hidden costs – just a flat fee. If your migraine medication runs $1,000+ per month without coverage, the math speaks for itself.
Appeal Timelines: How Long Does an Ubrelvy Appeal Take?
Submitting a complete, well-documented appeal from the start is the single best way to speed up the process. Incomplete submissions get delayed by requests for additional information. The average Claimable appeal gets a response in just 10 days.
FAQs
Why was my Ubrelvy denied if my doctor prescribed it?
A prescription and an insurance approval are two different things. Most plans require prior authorization for Ubrelvy, and those PA criteria often include step therapy requirements (trying triptans first), quantity limits, and documentation thresholds that go beyond what your doctor submits with a standard prescription. Your doctor determined Ubrelvy is right for you medically – the insurer is applying a separate, often more restrictive, set of criteria.
What if I can't take triptans — do I still have to try them before getting Ubrelvy?
No – and this is one of the strongest appeal arguments for Ubrelvy. If you have cardiovascular conditions that contraindicate triptans, or documented intolerance or side effects from prior triptan use, those count as "failure" under most step therapy policies. Your appeal should include specific documentation of why triptans are inappropriate for you. The insurer cannot require you to take a medication that your doctor has determined is medically unsafe.
Can I appeal an Ubrelvy denial myself, or does my doctor have to do it?
You can appeal yourself. Patient-initiated appeals carry their own legal protections – mandated response timelines, the right to escalate to external review, and multiple appeal levels. Your appeal is separate from anything your doctor's office files and doesn't depend on your doctor's appeal being successful.
Can I take Ubrelvy with an injectable CGRP medication like Aimovig or Emgality?
Published clinical evidence supports using Ubrelvy for acute treatment alongside a CGRP monoclonal antibody for prevention. They target different aspects of the CGRP pathway and serve different clinical purposes. If your insurer denied Ubrelvy based on "duplicate CGRP therapy," a clinical rationale from your neurologist citing the published safety data is typically the path to overturning it.
What's the difference between the 50mg and 100mg dose?
Both strengths are FDA-approved and showed similar pain freedom rates in clinical trials (21% at 2 hours for both 50mg and 100mg vs. 13% for placebo). For freedom from the most bothersome migraine symptoms – which includes nausea, sensitivity to light, and sensitivity to sound – rates were 38% for the 100mg tablet vs. 28% for placebo. The 100mg strength was also used in the PRODROME trial studying treatment during the early warning signs of a migraine and is often prescribed for patients with more severe attacks. Dose adjustments may also be needed based on other medications you take or kidney/liver function. If your insurer approved only the 50mg, your prescriber can submit a clinical rationale for the higher strength.
How many tablets of Ubrelvy should I be prescribed?
Ubrelvy's prescribing information establishes safety for treating up to 8 migraines per 30-day period, with the option for a second dose per attack. That means patients may need anywhere from 8 to 16 tablets per month depending on migraine frequency and whether a second dose is typically required. Insurer quantity limits vary: Some cap at 8 tablets, others at 10 or 16. If your prescribed quantity was denied, a quantity override request with clinical justification from your prescriber is the standard next step.
Is Ubrelvy the same as Nurtec?
No. Both are oral calcitonin gene-related peptide medications used in the treatment of migraines, but they're different drugs with different approvals. Ubrelvy (ubrogepant) is approved only for acute treatment, stopping a migraine attack in progress. Nurtec ODT (rimegepant) is approved for both acute treatment and prevention of episodic migraine. They also have different drug interaction profiles and dosing schedules. Other CGRP medications in the migraine landscape include Qulipta (atogepant), which is approved only for prevention, and Zavzpret (zavegepant), a nasal spray approved only for acute treatment. If your insurer wants you to switch to a different CGRP medication, your appeal should explain why Ubrelvy is the more appropriate choice for your specific situation.
How much does Ubrelvy cost without insurance?
The manufacturer's list price is approximately $1,085 for a month's supply. Retail prices can run higher, averaging around $1,300 for 10 tablets at some pharmacies. AbbVie offers the UBRELVY Complete Savings Card for commercially insured patients, which can reduce costs to as little as $0 per monthly fill (up to $7,000 in annual savings). Patients without commercial insurance who meet income requirements may qualify for AbbVie's patient assistance program (myAbbVie Assist), which provides the medication at no cost.
Is it worth appealing an Ubrelvy denial?
Absolutely. Insurers count on patients accepting a denial as final – fewer than 1% of denied claims are ever challenged. But appeals exist because denials are frequently wrong: documentation was incomplete, criteria were misapplied, or the insurer ignored clinical evidence. Your doctor prescribed Ubrelvy because you need it. The appeal is your opportunity to prove that case with the right evidence, the right arguments, and the right legal framework behind you.
Claimable's physician-led team has helped patients recover millions in care access by fighting insurance denials. We're SOC 2 Type II certified and HIPAA compliant. Learn more about how Claimable works →
Related: Why Was My Migraine Treatment Denied? Common Insurance Denial Reasons and How to Fight Back

Your doctor prescribed Nurtec ODT because it's the right treatment for your migraines. Your insurer said no. But you don't have to just give up on Nurtec. If it's the right treatment for you, let's talk about how to get covered.
Nurtec ODT is the only oral CGRP medication approved by the FDA for both treating acute migraines and preventing them. That dual role is a genuine clinical advantage, and it's precisely what makes the insurance process so frustrating. Insurers may apply different criteria depending on whether your doctor prescribed Nurtec for acute use, preventive use, or both, and many patients (and even some prescribers) don't realize the way the prescription is written directly determines which criteria the insurer evaluates.
Here's what Pfizer's own data says: 97% of patients with commercial insurance have plans that cover Nurtec ODT. If you were denied, that means that there's likely a path to getting covered through an appeal — whether it's through demonstrating that you meet the criteria, updating paperwork, or proving you deserve an exception to their rules.
If you're denied Nurtec, you can appeal
Fewer than 1% of denied claims are ever appealed. Insurance companies count on that. But when patients do appeal with the right evidence, they often win. At Claimable, we see this in practice — with over 80% of our appeals getting approved in established conditions.
This guide walks you through exactly why your Nurtec coverage was denied, how to identify your specific denial type, and what a winning appeal actually looks like, including the timelines, documentation, and strategies that work.
Why Insurance Companies Deny Nurtec Coverage
Understanding the specific reason for your denial is the single most important step before doing anything else. The denial reason determines your entire strategy, and getting it wrong means wasting time on arguments that won't work for your situation.
What Makes Nurtec Denials Uniquely Complicated
Most migraine medications do one thing: treat an attack or prevent future ones. Nurtec does both. That's a significant clinical advantage, but it creates a coverage problem that doesn't exist with drugs like Ubrelvy (acute only) or Qulipta (prevention only).
If your doctor prescribed Nurtec for acute use, the insurer applies one set of criteria, typically requiring you to have tried and failed triptans first. If prescribed for prevention (every-other-day dosing), the insurer applies a different, often stricter set of criteria — requiring documented failure of older preventive drugs like beta-blockers, antidepressants, or antiepileptics.
If your doctor intended Nurtec to serve both roles, the prior authorization may need to address both sets of requirements simultaneously. Many prescribers don't realize this, and many PAs are submitted addressing only one indication.
The quantity of tablets prescribed can also trigger a denial. Preventive dosing requires roughly 15 tablets per month, while acute use calls for up to 8. A prescription for 15 tablets submitted with acute-only documentation will get flagged immediately.
The mismatch between how the prescription is written and what the insurer's criteria require is one of the most common, and most preventable, reasons Nurtec gets denied.
The Most Common Types of Nurtec Denials
Most articles list denial types using the language insurers put in their letters. We think about denial types based on what they actually mean for patients and how they shape your strategy.
Step Therapy Required
This is the most common Nurtec denial. Insurers require patients to try and fail older medications first — especially triptans — before approving Nurtec, even when your doctor has clinical reasons for prescribing it first.
For acute use, most plans require documented failure of two or more triptans (sumatriptan, rizatriptan, zolmitriptan, eletriptan). For preventive use, the bar is even higher — many plans require failure of medications from two or more drug classes: beta-blockers (propranolol, metoprolol), antidepressants (amitriptyline, venlafaxine), antiepileptics (topiramate, valproate), or other CGRP therapies.
What most patients don't realize: "Failure" doesn't mean the drug didn't work. Side effects, contraindications, and medical reasons a drug is inappropriate also count as failure. For example, many patients with cardiovascular disease can't safely take triptans, which means insurers should not require them to try these medications first.
Important: The American Headache Society's 2024 position statement explicitly recommends CGRP-targeting therapies — including Nurtec — as a first-line option for migraine prevention, without requiring prior failure of older drug classes. When an insurer demands you fail on beta-blockers or topiramate before accessing Nurtec, they're contradicting the leading medical society's guidance. That's a powerful argument in any appeal.
Not Medically Necessary
This denial often means the initial submission was too thin, not that your insurer reviewed your full history and determined Nurtec isn't appropriate. Common gaps: not specifying migraine frequency, not listing comorbidities, not documenting impact on daily functioning, or not explaining why Nurtec specifically is the right choice.
A Nurtec watch-out: Because the drug is approved for both acute and preventive use, the prescriber needs to clearly document which indication is being requested and why. A submission that doesn't specify this can trigger a medical necessity denial even when you need it.
Quantity Limit Exceeded
Many insurers set a default quantity limit of 8 tablets per month, aligned with acute use. If your doctor prescribed Nurtec for prevention (roughly 15 tablets per month), the prescription may automatically get flagged.
This is often a straightforward fix: your prescriber submits documentation confirming the preventive indication and requests a quantity override. But the quantity limit PA criteria are often separate from the initial coverage PA, so you may need to clear two hurdles, not one.
Not on Formulary / Non-Preferred Brand
Some plans prefer a different CGRP medication — often Ubrelvy for acute use, or Qulipta, Aimovig, Emgality, or Ajovy for prevention. This isn't a medical judgment about whether you need the medication, it's a business decision about which drugs the insurer has negotiated pricing for.
The strongest argument centers on Nurtec's dual indication. If your doctor prescribed it for both acute treatment and prevention — which no other oral CGRP medication can do — replacing it with two separate drugs increases complexity, cost, and adherence burden. That's a compelling case for a formulary exception.
PA Requirements Not Met
This denial means the insurer believes one or more coverage criteria weren't satisfied. In many cases, the issue isn't that you actually fail the criteria — it's that the insurer applied the rules incorrectly, ignored clinical details, or relied on outdated requirements.
Common scenarios: migraine frequency disputes (your documented frequency meets the threshold but wasn't clearly presented), indication mismatch (the PA was submitted for one indication but the quantity suggests another), or incomplete treatment history (the documentation didn't fully capture your prior medication trials).
Incorrect Diagnosis Code
Coverage often hinges on submitting the correct ICD-10 diagnosis code. Common issues include using a general headache code instead of a specific migraine code, or failing to specify episodic migraine when requesting preventive coverage. Pfizer's own resources flag incorrect codes as one of the most common reasons for Nurtec PA denials. This is often the easiest denial to fix.
A breakdown of common ICD-10 diagnosis codes for migraine treatment:
Duplicate CGRP Therapy Denial
If you're already taking an injectable CGRP (Aimovig, Ajovy, or Emgality) for prevention, some insurers will deny Nurtec for acute use, claiming you can't use two CGRP drugs at the same time. This denial is often wrong — the American Headache Society and published clinical evidence support using a CGRP monoclonal antibody for prevention alongside an oral gepant for acute treatment, because they work through different mechanisms. Overturning this typically requires a detailed clinical rationale from a neurologist or headache specialist.
How to Appeal a Nurtec Denial: Step by Step
Appeals work far more often than most people think. The insurance industry has spent decades conditioning patients to accept "no" as final. It's not.
Step 1: Read Your Denial Letter Carefully
Your denial letter is required by law to include the specific reason for denial, your appeal rights, and the deadline to file.
Find your deadline. Most commercial plans allow 180 days, but deadlines vary significantly by insurer. UnitedHealthcare gives you just 65 days for most plan types — less than half the time Aetna, BCBS, and Cigna allow. Medicare Advantage plans follow CMS guidelines of 60 days. Missing the deadline means you won't be allowed to appeal, so move as quickly as possible.
Step 2: Understand That You Can Appeal, Not Just Your Doctor
You can file an appeal yourself, as the patient, separate from (or in addition to) your doctor filing a provider-level appeal. Patient-initiated appeals often have stronger legal protections than provider appeals — including mandated response timelines, the right to escalate to an independent external reviewer, and multiple levels of appeal. If your doctor's prior authorization or appeal was denied, that doesn't mean yours will be. They're different processes.
Step 3: Clarify the Prescription With Your Doctor
Before gathering documentation, confirm with your prescriber: Was Nurtec prescribed for acute treatment, preventive treatment, or both? Was the PA submitted with the correct indication and quantity? Were the correct ICD-10 migraine codes used?
If the issue is a mismatch between the prescription and the PA submission, a corrected resubmission may resolve the denial without a formal appeal.
Step 4: Get a Letter of Medical Necessity
A letter of medical necessity (LOMN) from your prescribing physician is the single most important document in a Nurtec appeal. It should include documentation of your migraine days per month, prior medication history and diagnosis code.
How to ask your doctor: Be direct. "My insurance denied Nurtec. Would you be willing to write a letter of medical necessity for my appeal? I can bring information on what the insurer typically looks for." Some doctors aren't experienced with writing these, but offering a template or outline can help significantly.
Step 5: Build Your Appeal Package
Your appeal should include a cover letter summarizing your case, the letter of medical necessity from your doctor, supporting clinical documentation (records showing migraine frequency, treatment history, comorbidities), and a personal statement explaining how the denial affects your health and daily life.
The three pillars of a winning appeal:
- Your story — the personal health impact of this denial
- Clinical evidence — studies, guidelines, and medical records supporting Nurtec for your situation
- Policy and legal analysis — how your situation meets coverage criteria under your plan, state law, and federal regulations
Step 6: Submit and Track
Submit your appeal per the instructions in your denial letter. Your insurer is required to respond within 30 days for standard appeals, or 72 hours for urgent/expedited cases. Keep records of when you submitted, how (fax, mail, portal), and any confirmation numbers.
Step 7: Escalate If Needed
If your internal appeal is denied, you have the right to an external review by an independent third party not employed by the insurer. External reviews commonly overturn denials that make it to that stage — because the reviewer evaluates whether the denial was medically justified, not whether the insurer wants to pay.
Don't give up after one "no." The system is designed to make you quit. Persistence is part of the strategy.
An Easier Path: Let Claimable Handle Your Nurtec Appeal
If navigating this process feels overwhelming, or if you just don't have time to become an expert in insurance appeals, Claimable can help.
Here's how it works:
- Answer a few questions about your Nurtec denial and medical history
- We build your case using our database of 4+ million clinical studies, insurer policies, and legal standards
- We create a fully customized appeal with your personal story + clinical evidence + policy analysis
- We submit it for you, faxed and mailed directly to your insurer
- We guide you through escalation if needed
80%+ of Claimable appeals succeed, with most resolved in 10 days or less.
"When my insurance company denied my claim to continue with my medicine, I felt defeated at first... Then I found Claimable. In the end I ended up winning my claim and I couldn't have done it without Claimable. I highly recommend them." — April A.
Appealing with Claimable is just $39.95. No success fees, no hidden costs. Just a simple flat fee. If your migraine medication costs $1,000+ per month, the math is simple.
Appeal Timelines: How Long Does a Nurtec Appeal Take?
The faster you submit a complete, well-documented appeal, the faster you'll get a decision. While these timelines seem slow, getting your appeal right can speed things up significantly. The average Claimable appeal gets a response in just 10 days.
FAQs
Why was my Nurtec denied if my plan covers it? Having Nurtec on your plan's formulary doesn't mean it's automatically approved. Most plans require prior authorization, and the PA criteria often include step therapy requirements, quantity limits, or documentation thresholds that aren't obvious from your benefits summary. Pfizer reports that 97% of commercial plans cover Nurtec — but "covered" and "approved without a fight" are very different things.
Can I appeal a Nurtec denial myself, or does my doctor have to do it? You can appeal yourself. Patient-initiated appeals often have stronger legal protections than provider appeals, including mandated timelines and the right to external review. You can appeal in addition to your doctor's appeal — they're separate processes.
What if my insurer wants me to try Ubrelvy instead of Nurtec? This is a step therapy requirement. Your appeal should focus on why Nurtec specifically is the right choice. If you need both acute and preventive coverage, Nurtec is the only oral gepant approved for both — that's a strong clinical argument against switching to a drug that only covers one indication.
How many tablets should I be prescribed? For acute use, up to 8 tablets per month. For prevention, approximately 15 tablets per month (75 mg every other day). The maximum is 18 doses in a 30-day period. If your doctor prescribed preventive dosing, make sure the PA was submitted for the preventive indication.
Can I take Nurtec with an injectable CGRP medication like Aimovig? Some insurers will deny this combination, but clinical evidence and AHS guidance support using a CGRP monoclonal antibody for prevention alongside an oral gepant for acute treatment. If you receive a duplicate therapy denial, a detailed clinical rationale from your neurologist is essential.
What's the difference between Nurtec and other CGRP medications? CGRP medications aren't interchangeable. Nurtec is the only oral gepant approved for both acute treatment and prevention of episodic migraine. Ubrelvy and Zavzpret are acute-only. Qulipta is prevention-only. Aimovig, Ajovy, Emgality, and Vyepti are injectable monoclonal antibodies for prevention.
How much does Nurtec cost without insurance? Approximately $1,000+ for an 8-tablet dose pack. Pfizer offers a savings card for commercially insured patients that can reduce the cost to as little as $0/month (with a $7,000 annual cap), and a first-fill program providing one prescription at no cost while benefits are verified.
Is it worth appealing? Yes. The insurance industry counts on patients giving up — fewer than 1% of denials are ever appealed. But when patients do appeal with proper documentation, overturn rates are significant. You've already been prescribed this medication by a doctor who believes you need it. The appeal is your chance to make that case.
Claimable's physician-led team has helped patients recover millions in care access by fighting insurance denials. We're SOC 2 Type II certified and HIPAA compliant. Learn more about how Claimable works →
Related: Why Was My Migraine Treatment Denied? Common Insurance Denial Reasons and How to Fight Back

Your doctor prescribed Zepbound because you need it. But your insurance said no. When it comes to GLP-1s, this is unfortunately common.
If you've been denied coverage for Zepbound, you're far from alone. According to the 2025 KFF Employer Health Benefits Survey, only about 19% of large employer plans cover GLP-1 medications for weight loss. That means that the majority of people seeking Zepbound coverage will hit a wall before they even get started.
Here's what most people don't realize: the word "denied" doesn't always mean the same thing. A "forced switch" denial (where your insurer wants you to take Wegovy instead, for example) requires a completely different response than a blanket "weight loss drugs aren't covered" exclusion. Most online advice lumps these together and offers generic tips, which can waste your limited chances to overturn the decision.
The insurance industry is counting on you not knowing the difference. They're also counting on you giving up. Another KFF analysis found that fewer than 1% of denied claims are ever appealed. Yet when patients do appeal with the right evidence, the results can be dramatic. At Claimable, we see this in practice every day – with over 80% of our appeals getting approved in established conditions.
This guide walks you through exactly why your Zepbound coverage was denied, how to identify your specific denial type, and what a winning appeal actually looks like – including the timelines, documentation, and strategies that work.
Why Insurance Companies Deny Zepbound Coverage
Understanding the specific reason for your denial is the single most important step before doing anything else. The denial reason determines your entire strategy – and getting it wrong means wasting time on arguments that won't work for your situation.
The Real Breakdown: What We See in Thousands of Zepbound Appeals
Most articles list denial types alphabetically, or using the language that the insurer uses in their letters. We think of denial types based on what they mean for patients and how they influence how you fight back. Here's what actually happens, based on the Zepbound appeals we handle:
Forced Switch Denials
This is what we see most often. Your insurer isn't saying Zepbound isn't working for you – they're saying they'd rather pay for something else.
The argument that wins: Clinical differentiation and previous failures. Zepbound is a dual GIP/GLP-1 receptor agonist. Wegovy is GLP-1 only. If you've responded well to Zepbound, or if you tried semaglutide-based medications previously without adequate results, that's your leverage.
Document: your response to Zepbound, any previous experience with other GLP-1s, side effects you experienced on alternatives, and your prescriber's clinical rationale for why Zepbound specifically is the right choice.
Not on Formulary Denials
Every plan has a list of "preferred" drugs, and yours doesn't include Zepbound. This isn't a medical judgment about whether you need the medication – it's a business decision about which drugs the insurer has negotiated pricing for.
The argument that wins: Request a formulary exception. Insurers are required to have a process for covering non-formulary drugs when there's a valid medical reason. Your case is stronger if you can show that formulary alternatives (like Wegovy) aren't appropriate for you – whether because you've tried them without success, experienced side effects, or have a clinical profile that makes Zepbound the better choice.
Document: why the formulary alternatives don't work for your situation, your prescriber's rationale for Zepbound specifically, and any clinical evidence supporting tirzepatide over semaglutide-based options for patients like you.
Blanket Plan Exclusion Denials
These are the toughest. Your plan has decided, as a matter of policy, not to cover weight loss medications. That's not a medical judgment you can argue against — it's a plan design choice.
Your options:
For employer-sponsored plans: Go through HR. Many employers don't realize their plan excludes these medications, or they're open to reconsidering. Frame it as a healthcare equity and outcomes issue.
Explore the OSA indication: Zepbound is FDA-approved for moderate-to-severe obstructive sleep apnea in adults with obesity. If you have OSA (even if undiagnosed — it's extremely common in people with obesity), this indication may be covered even when "weight loss" isn't.
Out-of-plan options: Manufacturer savings programs, cash-pay pharmacies, or alternative coverage may be worth exploring while you work on the appeal.
Not Medically Necessary Denials
This denial often means the initial submission was too thin. Insurers look for specific documentation, and if it's not there, they deny.
What a strong submission includes:
- Current BMI and weight history
- Complete list of comorbidities (hypertension, sleep apnea, prediabetes, PCOS, joint problems, NAFLD, etc.)
- Documentation of previous weight loss attempts (diet programs, exercise regimens, prior medications)
- Lab work supporting metabolic dysfunction
- Clinical rationale for why Zepbound is appropriate for this specific patient
If your initial prior authorization was bare-bones, appealing or resubmitting with complete documentation can flip the outcome.
Step Therapy Denials
Your insurer wants you to try (and fail on) other medications before they'll approve Zepbound. The most common requirements: Wegovy, Saxenda, Contrave, or metformin (for patients with prediabetes or insulin resistance).
Two paths forward:
Complete the step therapy: If you haven't tried these medications, your insurer may have a point. Try them as prescribed, document the results, and resubmit.
Request a step therapy exception: If there's a clinical reason why the required alternatives aren't appropriate for you – prior adverse reactions, contraindications, or documented failure – your doctor can request an exception.
PA Requirements Not Met
This denial means the insurer claims you didn't meet one or more coverage requirements for the medication. These rules may include BMI thresholds, participation in a weight management program, trying other medications first, or demonstrating enough weight loss while on treatment. In many cases, the issue isn't that you actually fail the criteria—it's that the insurer applied the rules incorrectly, ignored important medical details, or relied on outdated assumptions about obesity treatment.
If your denial says prior authorization requirements weren't met, a well-supported appeal can often show that you do meet the criteria - or that the insurer applied them incorrectly.
A Note on Diagnosis Code Issues
This is more common than people realize. Zepbound is FDA-approved for chronic weight management (obesity) and for moderate-to-severe obstructive sleep apnea in adults with obesity. Mounjaro is the same active ingredient (tirzepatide) but approved for type 2 diabetes.
Coverage often hinges entirely on how the claim is coded. If you have multiple conditions, the diagnosis code your prescriber uses can make or break coverage. This is a conversation to have with your prescriber's office.
The Big One: CVS Caremark
If your Zepbound was denied by CVS Caremark, you're not imagining things. In the Zepbound appeals we've handled, CVS Caremark denials outnumber every other insurer and PBM combined.
The big reason for this? Their 2025 decision to drop Zepbound from their formulary in favor of Wegovy. Both drugs are GLP-1s, both help with weight management – so on paper, the switch looks reasonable. But Zepbound (tirzepatide) and Wegovy (semaglutide) work differently. Zepbound is a dual GIP/GLP-1 agonist; Wegovy targets only GLP-1. For some patients, that difference matters enormously.
If you've been stable on Zepbound and CVS Caremark wants to switch you to Wegovy, that's a legitimate clinical concern – and a strong foundation for an appeal.
Other major deniers we see: OptumRx, Express Scripts, Blue Cross Blue Shield (various plans), Anthem, Aetna, and UnitedHealthcare. FEP Blue also made significant formulary changes for 2026 that affect Zepbound coverage, pushing patients toward alternatives regardless of individual circumstances.
How to Appeal a Zepbound Denial: Step by Step
Appeals work far more often than most people think. The insurance industry has spent decades conditioning patients to accept "no" as final. It's not.
Step 1: Read Your Denial Letter Carefully
Your denial letter is required by law to include: the specific reason for denial, your appeal rights, and the deadline to file.
Find your deadline. Most commercial plans allow 180 days, but deadlines vary significantly by insurer. UnitedHealthcare gives you just 65 days for most plan types – less than half the time Aetna, BCBS, and Cigna allow. Medicare Advantage plans follow CMS guidelines of 65 days. Missing the deadline means you won't be allowed to appeal, so we always recommend moving as quickly as possible.
Step 2: Understand That You Can Appeal (Not Just Your Doctor)
Here's something most articles miss entirely: you can file an appeal yourself, as the patient, separate from (or in addition to) your doctor filing a provider-level appeal.
Why this matters: Patient-initiated appeals often have stronger legal protections than provider appeals. You have mandated response timelines, the right to escalate to an independent external reviewer, and multiple levels of appeal. Providers filing on your behalf don't always have these same protections.
If your doctor's appeal was denied, that doesn't mean yours will be. They're different processes.
Step 3: Get a Letter of Medical Necessity
This is your primary weapon. A letter of medical necessity (LMN) is a formal document from your prescribing physician explaining why Zepbound is required for your specific medical situation.
What a strong LMN includes:
- Your diagnosis codes (ICD-10) and clinical history
- BMI, weight trajectory, and documented comorbidities
- Summary of previous treatments attempted and why they were insufficient
- Clinical studies supporting tirzepatide's efficacy (citing SURMOUNT-1 or SURMOUNT-2 trials is helpful)
- Explanation of why alternatives aren't appropriate for you specifically
- Reference to your insurer's own coverage criteria and how you meet them
How to ask: Be direct with your doctor. "My insurance denied Zepbound. Would you be willing to write a letter of medical necessity for my appeal? I can provide information on what the insurer typically looks for."
Some doctors aren't familiar with writing these. You can offer to bring a template or outline.
Step 4: Build Your Appeal Package
Your appeal should include: a cover letter stating your request and summarizing your case, the letter of medical necessity from your doctor, supporting clinical documentation (labs, records showing comorbidities, weight history), a personal statement explaining how the denial affects your health and daily life, and any relevant clinical studies or guidelines supporting Zepbound for your condition.
The three pillars of a winning appeal:
- Your story – the personal health impact of this denial
- Clinical evidence – studies, guidelines, and medical records supporting the treatment
- Policy and legal analysis – how your situation meets coverage criteria under your plan, state law, and federal regulations
Step 5: Submit and Track
For internal appeals: Submit to your insurer per the instructions in your denial letter. They're required to respond within 30 days for standard appeals (72 hours for urgent/expedited appeals).
Keep records: Document when you submitted, how (fax, mail, portal), and any confirmation numbers. Insurers lose things. Having a paper trail protects you.
Step 6: Escalate If Needed
If your internal appeal is denied, you have the right to an external review by an independent third party not employed by the insurer.
External reviews overturn roughly 40% of denials that make it to that stage. The reviewer isn't on the insurer's payroll – they're evaluating whether the denial was medically justified.
Other escalation options:
- File a complaint with your state's Department of Insurance
- For employer-sponsored ERISA plans, you may have additional legal options
- For federal employee plans (like FEP Blue), you can escalate to the Office of Personnel Management
Don't give up after one "no." The system is designed to make you quit. Persistence is part of the strategy.
How Long Does a Zepbound Appeal Take?
In the Zepbound appeals we handle, the median resolution time is 6 days. Most cases resolve quickly, but know that there's a long tail of complex cases that can stretch longer.
Industry & legal timelines:
- Internal appeals: Insurers must respond within 30 days (72 hours for urgent cases, like a forced switch)
- External reviews: Typically 45-60 days
- Full process (internal + external): 6-10 weeks if you go through both stages
The faster you submit a complete, well-documented appeal, the faster you'll get a decision. In some cases, Claimable automatically submits appeals to both internal and external review at the same time to speed up the process.
Real Zepbound Appeal Wins
People often think "denied" means "will never be covered". With the thousands of Zepbound appeals we've handled, we're here to tell you that you absolutely can get coverage back. Here are some stories from real patients.
"Claimable is an amazing service. They helped me get my Zepbound appeal overturned. Anytime I had a question the response was very fast and detailed. I highly recommend them. It's worth every dollar you spend." — Chante W.
"I cannot thank the Claimable team enough. They led me through the process, took me to third and final outside appeal process. Guided me personally, took the time to help, and the end result was victory over CVS Caremark. I am now back on Zepbound, a drug that has changed my life, and 100% paid for by my insurance carrier." — John C.
"So grateful to have found Claimable through On The Pen with Dave Knapp. I had read about how Claimable has helped others with prior authorization. I admit I was skeptical, but not being able to get Zepbound approved for my obstructive sleep apnea was so frustrating. I bit the bullet went to their site and began the appeal process. The staff at Claimable… were quick to reply to questions as well as suggestions on how to succeed. I am happy to say the Zepbound was approved for one year and I am picking it up tomorrow." — Rita M.
An Easier Path: Let Claimable Handle Your Appeal
If navigating this process feels overwhelming, or if you just don't have time to become an expert in insurance appeals, Claimable can help.
Here's how it works:
- Answer a few questions about your Zepbound denial and medical history
- We build your case using our database of 4+ million clinical studies, insurer policies, and legal standards
- We create a fully customized appeal: your personal story + clinical evidence + policy analysis
- We submit it for you: faxed and mailed directly to your insurer
- We guide you through escalation if needed
We've handled thousands of Zepbound cases, so we know which arguments work with which insurers, what to escalate and when, and are here to help you through any questions you may have.
Appealing with Claimable is just $39.95. No success fees, no hidden costs. Just a simple flat fee. If your medication costs $1,000+ per month, the math is simple.
FAQs
Why was my Zepbound denied? The most common reasons are forced switches (your insurer prefers Wegovy), formulary exclusions, blanket anti-obesity medication exclusions, insufficient documentation, and step therapy requirements. Your denial letter should specify the reason – that determines your appeal strategy.
Can I appeal a Zepbound denial myself, or does my doctor have to do it? You can appeal yourself. In fact, patient-initiated appeals often have stronger legal protections than provider appeals, including mandated timelines and the right to external review. You can appeal in addition to your doctor's appeal – they're separate processes.
What's the difference between Zepbound and Mounjaro? Same active ingredient (tirzepatide), different FDA approvals. Zepbound is approved for chronic weight management and obstructive sleep apnea in adults with obesity. Mounjaro is approved for type 2 diabetes. Coverage often depends on which diagnosis code is submitted.
How long do I have to appeal? Most commercial plans allow 180 days, but some insurers have shorter deadlines (60-65 days for some UnitedHealthcare plans, for example). Check your denial letter for your specific deadline.
What if my doctor's prior authorization was denied? A denied prior authorization isn't the end. You can file a patient-initiated appeal, ask your provider to request a peer-to-peer review (where your doctor speaks directly with the insurer's medical reviewer), or resubmit with stronger documentation.
Is it worth appealing? Yes. The insurance industry counts on patients giving up – fewer than 1% of denials are ever appealed. But when patients do appeal with proper documentation, overturn rates are significant. You've already been prescribed this medication by a doctor who believes you need it. The appeal is your chance to make that case.
Claimable's physician-led team has recovered over $30 million in care value for patients facing insurance denials. We're SOC 2 Type II certified and HIPAA compliant. Learn more about how we work →

Dr. Warris Bokhari, Co-Founder and CEO of Claimable, was named to the 2026 TIME100 Health List of the World's Most Influential Leaders in Health. The annual list celebrates innovators and pioneers working to build healthier populations around the world.
The recognition is truly meaningful. And for those of us building alongside Warris, it reflects something we've seen up close for years — steady advocacy, rigorous thinking, and a deep commitment to standing up for patients when it matters most.
We wanted to take a moment to share more about the person behind the recognition and the principles that guide his work.
A path shaped by lived experience
Warris’s work has always been personal.
He was raised in England by two parents living with long-term disabilities. His mother lived with severe rheumatoid arthritis, and his father retired when Warris was still a child because of chronic back problems. Affordable, guaranteed access to healthcare wasn’t an abstract concept in their household — it was a daily reality, directly influencing stability, opportunity, and quality of life.
That experience stayed with him. Warris trained and practiced as a physician in the UK before moving to the United States, where he later held leadership roles across major healthcare and technology organizations, including GE Healthcare, Amazon, Apple, and Anthem.
Over time, he developed a clear-eyed view of how modern U.S. healthcare actually functions — not as a system optimized for care, but as one structured around financial risk, complexity, and friction — a stark contrast to the system he experienced growing up in the U.K.
Again and again, he saw the same outcome: patients prescribed necessary care, only to face delays or denials driven more by financial incentives than medical judgment.
Why Claimable exists
Claimable was born from that inequity. Warris didn’t set out to build a healthcare company. He set out to address an escalating crisis and change what happens when patient care collides with a system built around cost control.
He brought together co-founders Alicia Graham and Zach Veigulis around a clear conviction: patients deserve real support in those moments — not more paperwork, not more waiting, and not a process designed to wear them down. From the beginning, Claimable has been built on a simple principle: patients shouldn’t have to become experts, advocates, or adversaries just to access care.
For Warris, that means not only building tools that support patients at scale, but stepping in personally when the stakes demand it.
The cases people never see
Some of the most meaningful advocacy Warris does happens out of view, supporting patients in situations where access to care is genuinely life-or-death. This includes complex organ transplant denials and advanced oncology cases, where clinical nuance, timing, and judgment matter deeply.
In many of these cases, Warris has taken the lead, navigating the medical complexity and policy reasoning that ultimately shape critical coverage decisions. Being directly involved in these moments has been both sobering and instructive, reinforcing how much responsibility comes with building in this space.
That hands-on engagement doesn’t just shape his perspective — it informs our research and development efforts, pioneering strategies in new conditions and therapies before translating them into tools within Claimable. It has pushed the boundaries of what we believe can be done at scale by combining clinical rigor with purpose-built technology. And it continually sharpens our understanding of what good judgment looks like under pressure.
“I’ve worked closely with Warris on some of the most difficult cases we’ve encountered. What stands out is his steadiness — knowing when to push, when to pause, and how to carry the weight of decisions that affect real lives.” — Zach Veigulis, Co-Founder & CAIO, Claimable
Real Patient Impact
Take the story of Keaton, a 35-year-old father who was diagnosed with Stage IV bile duct cancer confined to his liver. After an extensive multidisciplinary review, he had been fully cleared for a transplant at Houston Methodist. Despite being his only potentially curative option, the transplant was denied, effectively forcing Keaton toward palliative care.
His wife, Tori, posted online asking for help, and Warris didn’t hesitate. He stepped into one of the most complex and visible cases imaginable, not because it was easy, but because it was right.
Warris immersed himself in the clinical research, the transplant criteria, and the insurer’s policy language — and just as importantly, in Keaton’s story. He got to know the family. He understood what was on the line.
Keaton later wrote, “I honestly might not be alive today if it weren’t for Warris and the team. They are highly knowledgeable and genuinely want to help people. I would recommend them to anyone and everyone if you’re having issues with insurance or being denied a life-saving treatment like I was.”
Keaton’s story isn’t unique in Warris’s world. It’s representative of the calls he answers every day — quietly, urgently, and when the outcome matters most.
Advocate first, CEO second
Warris has always led as an advocate first: for patients, for providers, and for the integrity of medicine itself. Inside the company, that philosophy becomes culture.
He stays closely connected to the lived reality of navigating denials and keeps the urgency of this mission front and center. Whether cold-calling early provider partners, supporting families facing devastating denials, or digging into emerging research on new therapies, he sets the tone for how we operate.
Leading by example, Warris encourages us to be bold in our convictions, resourceful in our approaches, and unwavering in our integrity. That mindset has led to clear non-negotiables for Claimable: the patient story must be central; evidence must be expert-curated and accurate; patients’ rights must be defended, not sidelined; and there must always be a next step.
“I’m honored to work alongside Warris, who is a doctor by training and by creed — someone who takes ‘do no harm’ seriously in every interaction. He reminds all of us that this work is about more than overturning denials. It’s about restoring trust.” — Alicia Graham, Co-Founder & COO, Claimable
Warris’s recognition on the TIME100 Health list reflects years of difficult, often invisible work, and reinforces why Claimable exists in the first place. The lessons learned alongside individual patients continue to shape how we build — embedding empathy, rigor, and real-world insight into tools designed to support patients at scale. We’re incredibly proud of Warris for this well-deserved recognition. And we’re even more committed to the journey ahead.

Your medication worked. Your doctor prescribed it. And now your insurance says it's not covered.
Learning that your insurance plan doesn't cover your treatment is frustrating, and often leaves folks with a lot of questions. Whether you got a letter in the mail or a message from your doctor's office, you're probably wondering – what in the world is a formulary, and what do I do if my drug isn't on it?
A formulary is the list of drugs that are covered by your insurance plan. But what most people don't know is that even if your treatment isn't on the list, you can still get covered. Most plans are required to maintain a formulary exception process, and if that's denied, you have the right to appeal.
And when a formulary exception is granted, it means your insurance has to cover your treatment again – even if it's not on their official list.
Let's break down what to do if your med is "not on formulary", and how to get it covered again.
How to get a non-formulary drug covered: Quick answer
To get a non-formulary drug covered, request a formulary exception from your plan. Start by confirming why you were denied: Check your plan's formulary and get the denial reason in writing. Then, submit the exception request to your insurance. Ask your doctor for a letter of medical necessity to support your request, and clearly document any failed alternatives or other reasons why you need the exception. If your exception is denied, you have the right to appeal – and appeals supported by strong clinical evidence, legal citations, and a clear patient narrative succeed far more often than most people realize.
What Is a Formulary – and What Does "Not on Formulary" Mean?
A formulary or drug list is your insurance plan's list of approved medications. It's organized into tiers – typically ranging from low-cost generics to high-cost specialty drugs – and it determines what your plan will cover and at what cost.
When your drug is "not on formulary," it means your plan has decided not to include it on that list. When it's "non-preferred," it means they'll technically cover it, but only after you've jumped through additional hoops (usually trying cheaper alternatives first).
Here's the part most people don't realize: formularies aren't just about if a medication works. They're heavily influenced by rebate deals between insurers, pharmacy benefit managers (PBMs), and drug manufacturers. A drug can be clinically effective, widely prescribed, and still get dropped from a formulary due to behind-the-scenes business deals. The medication didn't change. The science didn't change. But the business math did.
That distinction matters, because it means a formulary exclusion is often a financial decision dressed up as a medical policy – and financial decisions can be challenged.
How Formulary Denials Happen
If you're reading this, it's probably because you got a letter, a notification, or a phone call that tells you your medication isn't covered. These notifications can come in different forms, and what you should do next depends on what you're dealing with. Find the one below that sounds like you.

You got a letter saying your medication is being removed from formulary. This is a prospective formulary change – your plan is dropping the drug on a future date. Insurers are supposed to send this 60 days in advance (though the notice is mailed 60 days ahead, that doesn't mean it arrives that early). You only get this notice if the insurer knows you're currently filling the medication. If you just switched plans or are newly prescribed the drug, you won't be notified.
You got a denial notification in your pharmacy or insurance app. A short message in your CVS, Walgreens, or insurer app telling you the claim was denied. These notifications are a starting point, but they're often frustratingly incomplete – a brief description without the full denial reason, the policy they applied, or your appeal rights. Don't assume this is the whole story.
You got a formal denial letter in the mail. This is the letter with the specific denial reason and information about your rights. It's the most complete notification – but it can take two to four weeks to arrive after the initial denial. That's weeks you could be using to prepare.
Your doctor or pharmacist told you it's not covered. Sometimes your provider checks your benefits, sees the drug isn't on formulary, and tells you they're going to switch you to something else. In this scenario, you may not receive a formal denial at all. If this happens, it's worth having a conversation with your provider about whether you want to switch, because you do have other options.
Regardless of how you found out: call your insurer and request the full documentation – the exact denial reason, the coverage policy they applied, and your appeal rights and process. Ask them to send it the fastest way possible: through your online portal, faxed to your provider who can share it with you, or emailed directly. Don't wait for paperwork to arrive on its own timeline. And don't wait for the formal denial letter to start preparing – you can begin gathering documents and building your case as soon as you know there's a problem.
The Biggest Misconception: "Not Covered" Doesn't Mean Final
The most common reaction when patients hear "not on formulary" is to assume there's nothing they can do. That it's a final decision — and that "not covered" means "can never be covered."
It's not. And this is perhaps the single most important thing to understand about the entire process.
Even many providers will tell patients "it's not covered, there's nothing we can do" – and that's simply not accurate. You have a legal right to request a formulary exception, and if that's denied, you have additional appeal rights including independent external review. Insurance companies benefit enormously from people believing that "not covered" is the end of the road. For the vast majority of denial types, it's actually the beginning.
A note on weight loss medications: If your medication is excluded specifically because your plan doesn't cover drugs for weight loss as a category, that's a plan exclusion – which is different from a formulary exclusion and significantly harder to fight. If you're in this situation, we've got a whole guide to plan exclusions here.
Formulary Exception vs. Prior Authorization: What's The Difference?
In many cases, you can't formally request an exception until there's a written denial. The PA is often what generates that denial.
What Is a Prior Authorization (PA)?
A prior authorization is when your insurer requires your doctor to request approval before a medication will be covered. Your doctor submits clinical documentation, and the insurer decides whether the drug meets the plan's coverage criteria.
A medication can be on the formulary and still require a PA. Many plans apply PA requirements to brand-name, specialty, or high-cost drugs.
If a drug is non-formulary (not on the approved drug list), coverage usually requires an exception review — and in most plans, that request is submitted through the same PA system. That's why the terms often get confused.
What is a Formulary or Medical Exception?
A formulary exception is a formal request to cover a drug that is not included on your plan's formulary. You're asking the insurer to make an exception based on medical necessity, failure of covered alternatives, lack of equivalent options, or risk of harm from switching.
How the process actually works
In many cases, you can't formally request an exception until there's a written denial. The PA is often what generates that denial.
If your current medication is removed:
Benefits are checked → A PA is required or the drug is non-formulary → A PA is submitted → The PA is denied → You request a formulary exception and/or file an appeal
If you're prescribed a new non-formulary medication:
The prescription is sent to the pharmacy → You're told it's not covered or needs a PA → A PA is submitted → The PA is denied → You request a formulary exception and/or file an appeal
If you're forced to switch and the new medication isn't working:
Your insurer requires you to switch to a covered alternative → You try the new medication → It's ineffective, causes side effects, or worsens your condition → Your provider submits a PA to return to the original medication → The PA is denied → You request a formulary exception and/or file an appeal
Why this matters: In all three situations, the prior authorization often generates the written denial that unlocks your right to appeal.
Insurance rules are layered and technical. Claimable helps you move from denial to action — so treatment decisions stay where they belong: between you and your doctor.
How to Request a Formulary Exception
Make sure you have an active denial
Before you can pursue a formulary exception, you generally need a current, documented denial.
If you've received notice that your formulary is changing on a future date, don't wait and hope it resolves itself. Ask your provider to submit a new prior authorization on the first day the change takes effect. Once the change is active, any prior approval is typically no longer valid — even if it feels like it should be.
Your provider may not automatically resubmit a PA, but they can. Just ask.
Once that new PA is denied, you have a clean, current denial to challenge.
Choose your pathway
There are two ways to pursue a formulary exception, and you can actually do both at the same time:
The provider pathway: Your doctor submits a formulary or medical exception request to your insurer, focused on clinical justification. This may include documentation showing that covered alternatives were ineffective (therapeutic failure), alternatives caused adverse effects (intolerance), and/or alternatives are unsafe due to contraindications or FDA warnings. This pathway centers on proving medical necessity.
The patient appeal pathway: You submit a formal patient appeal directly to your health plan. This is the pathway you control immediately. It allows you to go beyond clinical arguments and include how the denial personally impacts your health, life and finances and call out specific legal protections and policy inconsistencies that show your care should be covered. You can also attach your provider's medical justification.
You don't have to choose just one. Pursuing both pathways can increase your chances — think of it as "more shots on goal." If you're already researching on your own, we recommend starting a patient appeal – it puts more tools at your disposal and doesn't depend on your provider's timeline or capacity. Appeals are strongest when patients and providers work together.
A note on "formulary exception forms"
If you've been searching for a standard "formulary exception form," you're not alone. Most exception forms are designed for providers, not patients. And even when they exist, they often don't leave room to fully present your case — including clinical evidence, legal arguments, and policy support.
Don't get stuck form-hunting. You can submit a formal appeal letter directly to your plan's appeals department — or use Claimable to generate and submit the request for you. If your insurer needs additional clinical documentation, they can request it directly from your provider during the review process.
Use the right language
Here's what most guides won't tell you: the specific language you use can determine whether your request is properly categorized or quietly buried. Insurers route requests based on trigger words. If you don't explicitly ask for a "formulary exception" and state why you qualify, your request may be miscategorized as a general inquiry – which means longer timelines, less scrutiny, or it simply being ignored.
You qualify for a formulary exception under three main categories:
- Therapeutic failure – the formulary alternatives were tried and either never worked or stopped working over time. Be specific: name each medication, how long you were on it, and what happened.
- Adverse events – you experienced side effects that made the formulary alternatives intolerable. This includes reactions that led to hospitalization, allergic responses, or side effects that significantly impacted your quality of life.
- Clinical contraindication – the formulary alternatives are medically inappropriate for you. This could be due to drug interactions, an FDA black box warning for your specific situation, or a co-existing condition that makes the alternative unsafe.
State your category clearly and explicitly in your request. Don't make them guess.
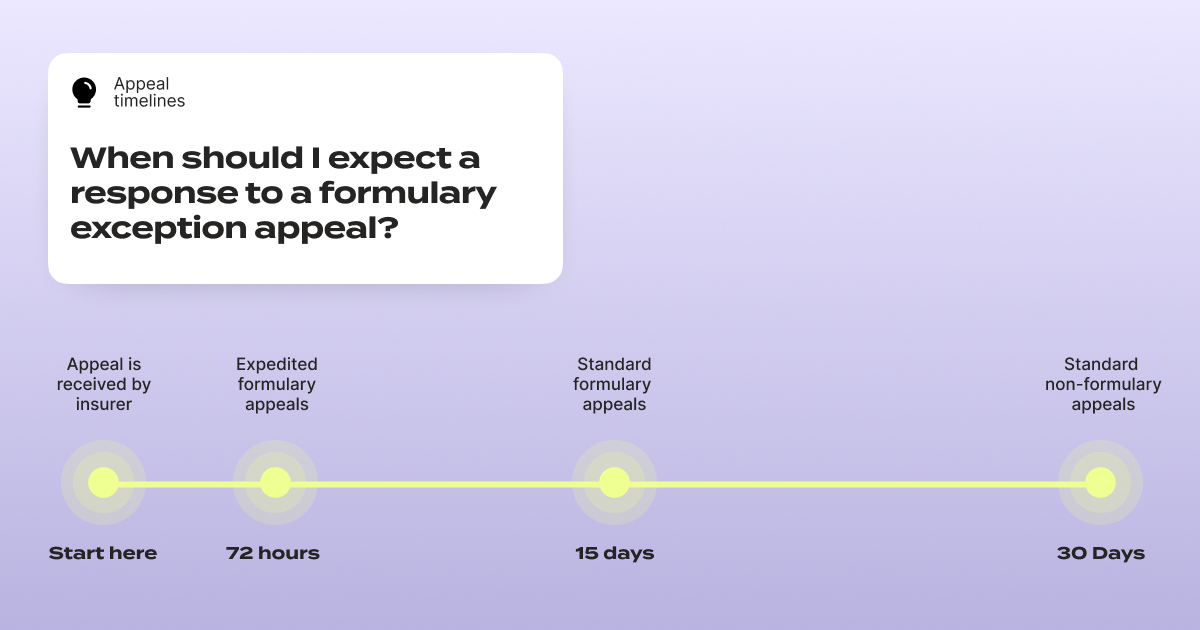
One critical timeline to know: under federal rules, insurers generally must provide expedited review within 72 hours for urgent requests and standard review within approximately 15 days for pre-service appeals – far faster than the standard 30-day review window for regular appeals.
But here's the catch: if you don't specifically request an expedited review and explain why your situation is urgent, many insurers will default to the standard timeline. If your health could seriously worsen by waiting, you have the right to request that 72-hour review. Put it in writing. At the very top of your appeal letter, write: EXPEDITED REVIEW REQUESTED (72 HOURS). Make sure it's impossible to miss.
Also double-check whether your insurer has a separate fax number or submission process for expedited appeals — they often do.
Know your rights, and state them clearly. Timelines vary by plan type, so always confirm your plan's specific rules.
Know Your Plan Type
Appeal rights and timelines can vary depending on your plan type and sponsor.
If you work for a large employer, you're likely on a self-funded plan, meaning your employer ultimately pays claims and serves as the plan fiduciary under the Employee Retirement Income Security Act (ERISA). In these cases, your appeal can reference your employer's duty to act in the best interests of employees.
Fully insured employer plans are generally subject to ERISA, the Affordable Care Act (ACA), and applicable state insurance regulations. Individual and exchange plans typically follow ACA and state rules. Federal and state employee plans, Medicare, and Medicaid each have their own appeal procedures and timelines.
Always review your plan documents — often called a Summary Plan Description (SPD), Evidence or Certificate of Coverage (EOC), plan brochure, or member handbook — to confirm the specific rules for formulary exceptions that apply to you.
What to Include in Your Formulary Exception Letter
A request that says "I need this medication" isn't enough. The ones that succeed build a structured case with specific, documented evidence. Here's what your letter should include:
The letter itself
Subject line: Request for formulary exception / appeal of non-formulary denial for [Drug Name]
Identify the denial. Your name, member ID (on your insurance card), date of denial, and the medication you were denied.
State what you're requesting. Be explicit: "I am requesting a formulary exception for [drug name], and coverage at the medically necessary level." Use the words "formulary exception." Don't leave room for miscategorization.
Explain why you need this specific drug. This is the core of your case:
- Your diagnosis and its severity, supported by test results or doctor's notes
- Why this drug is appropriate for your condition, citing clinical studies that support its effectiveness
- Why alternatives failed or are unsafe – name each one, how long you tried it, and what happened. If any alternatives carry warnings or contraindications for your situation, state that clearly.
- If you're stable on the drug: explain the improvement you've experienced and why switching creates risk – relapse, ER visits, loss of function, need for additional treatments. Spell out the real-world consequences rather than keeping it abstract.
Add legal and policy support. Reference applicable laws and protections – many states have laws against non-medical switching, and federal protections may apply depending on your plan type. If you're currently taking the medication and losing coverage could cause a gap in care, note this clearly and mark your request as "URGENT: Expedited review requested" to invoke the 72-hour review timeline.
Close with your ask and a list of supporting documents included.
And if you need help putting all of this together – that's where Claimable comes in. You answer some questions about the denial, your medical history, and personal story, and we get to work researching all the right studies, laws, and other evidence you need to build a strong appeal. Then, we fax and mail it for you. Our job is to translate your experience into a lawyer-level appeal letter, and give you the best possible chance of getting that exception approved.

The supporting documents (include as many as you have)
- Your denial documentation (notice letter, denial letter, portal screenshot or app screenshot)
- A Letter of Medical Necessity or the Medical Exception Form from your doctor
- A clear list of previously tried alternatives (drug name, dates, outcome, side effects)
- Relevant clinical notes from your medical records
- Any clinical studies supporting your medication for your condition
- A copy of your plan's rules, called a Summary Plan Description (SPD), Evidence or Certificate of Coverage (EOC), plan brochure, or member handbook
Where to find your clinical documentation: Your provider's patient portal is your best starting point (e.g., My Chart). Look for:
- Your medication list – showing what you've tried and why you stopped each one
- Your allergy list – documenting adverse reactions to specific drugs
- Visit notes from appointments where you and your provider discussed treatment decisions
If you can't find what you need in your portal, ask your provider directly for the clinical notes that document your treatment history – specifically the notes showing why alternatives failed or aren't appropriate for you.
Getting the Letter of Medical Necessity: If your provider is busy (and they always are), send them a template and specific talking points (we have one available here). Follow up – a single email that goes unanswered isn't enough when your coverage is on the line.
Common Mistakes That Waste Time or Hurt Your Request
Trying to resolve things by phone. Calling to check on the status of your request? Good to do, and can actually help – insurers have been known to claim they never received something until you provide tracking details (and then suddenly, they find it!). But don't try to appeal or negotiate a coverage decision over the phone. You don't want a low-level phone representative making decisions about your care. You want a written record, a formal process, and a qualified reviewer examining your evidence. Get everything in writing, ask them to send documentation of anything you discuss over the phone, and confirm everything they tell you in writing.
Filing a complaint with the wrong regulator. Many patients spend weeks drafting a complaint to their state Department of Insurance – only to learn that their plan is regulated at the federal level, where the state DOI has no jurisdiction. The majority of employer-sponsored plans are governed by federal law (ERISA), not state law. Before you spend time on a regulatory complaint, verify who actually regulates your plan. Your denial letter should include this information, or you can call your insurer and ask specifically: "Who handles external appeals for my plan?"
Not asserting your timeline rights. As mentioned above, formulary exceptions have faster review requirements than standard appeals. If you don't explicitly cite these timelines in your request, insurers have little incentive to prioritize it.
If Your Formulary Is Changing, Here's How to Prepare
If you've received notice that your medication is being removed from the formulary on a future date, don't wait for that date to arrive to take action.
- Get the longest supply you can now. If you're eligible for a 90-day fill, request it before the change takes effect. This gives you a buffer while you work through the exception and appeal process.
- Request a continuity of care exception. You can request a continuity of care exception to maintain coverage while your appeal is pending. Whether it is granted depends on your plan's rules, but it is absolutely worth asking.
- Have your provider file a new prior authorization on the first day the change takes effect. Your existing PA is effectively expired on the date the formulary change goes into effect, even though it shouldn't be. Your provider may not automatically resubmit a PA — but they can. Just ask. Once that new PA is denied, you have an active, current denial to appeal.
- Prepare your documentation in advance. Gather your clinical records, research the clinical evidence for your medication (or use Claimable to do the heavy lifting for you), and draft your personal statement. You don't want to be scrambling after you've been denied – you want to be ready to file immediately.
Don't Wait for the Denial Letter: Start Taking Action Immediately
You don't need to wait for the formal denial letter in the mail to start building your case. As soon as you know there's a problem – whether it's an app notification, a call from your pharmacist, or your doctor telling you they're switching your medication – make two phone calls.
Call your provider's office. Tell them you've been denied and you plan to challenge it. Ask for copies of the clinical notes that support your need for this medication – your treatment history, documentation of failed alternatives, and any relevant test results. Ask them to send it as quickly as possible.
Call your insurer. Request all documentation used to make the decision. Your denial letter (when it arrives) will likely include language stating you can request this – but you have to ask. Request:
- Clinical review notes
- Internal medical policies applied to your case
- Guidelines, criteria, or standards they relied on
- The name, credentials, and specialty of the reviewer
- Documentation of any automated systems or algorithms involved in the decision
Also file a separate claim file request – a formal request for your complete case file. This can take up to 30 days to fulfill (and insurers often don't comply unless you follow up), so getting it started immediately is smart. Consider sending it as a standalone request rather than bundling it with your appeal, since it may go to a different department.
Submit Your Appeal and Follow Up
Where to send it
Start with your denial letter or portal notice – it usually lists the appeals address, fax number, or portal upload path. If you don't see it, call the member services number on your insurance card and ask: "Where do I submit a member/patient appeal for a non-formulary denial?"
Some plans allow you to submit appeals through your online portal, which gives you a digital confirmation. If you fax, save the transmission receipt. If you mail, use certified mail with tracking.
When to follow up
If your appeal was faxed and the situation is urgent, call the next day to confirm they received it. If they say they don't have it, provide your fax confirmation details – they often "find" it once you can prove it was sent.
If your appeal was mailed, allow two to four weeks for delivery and processing. Once tracking shows it's delivered, start calling to confirm it's been logged and assigned for review.
Keep a simple log of every interaction: date, time, who you spoke with, what they said, and any reference numbers. This paper trail matters if you need to escalate.
What to Do If Your Formulary Exception Is Denied
A denied formulary exception is not the end. Your appeal rights include multiple levels of review, each with stronger protections – you can (and should!) keep fighting.
Request a second internal appeal. Your first step is a second internal appeal where a different reviewer – one who wasn't involved in the original decision – examines your case. Take a look at why they denied the request, add any additional evidence to support your case, and resubmit your appeal with REQUEST FOR SECOND INTERNAL REVIEW right at the top.
Escalate to external review. If your internal appeal is denied, you have the right to an independent external review – a decision made by a reviewer completely outside your insurance company. This is one of the strongest patient protections in the system, and insurers are bound by external review decisions.
Real Examples: Formulary Changes Happening Right Now
CVS Caremark dropping Zepbound for Wegovy
CVS Health announced that starting July 2025, Caremark would prioritize Wegovy on its standard formularies and drop Zepbound – tied to a partnership with Wegovy's manufacturer, Novo Nordisk. Patients who were stable on Zepbound were suddenly told they'd need to switch, regardless of how well the medication was working for them.
If you're in this situation, the playbook is exactly what we've described above: secure an active denial (via new PA), then submit a patient appeal showing why the forced switch isn't appropriate for you – including your treatment history, failed alternatives, and the real-world consequences of switching.
BCBS FEP Dupixent Formulary Changes
In November, BCBS FEP Blue announced that Dupixent would no longer be on their formulary. Some FEP Blue plans use a closed formulary, meaning if Dupixent isn't on the list, you pay the full cost unless you win an exception. Dupixent is a popular drug used for a wide range of conditions like atopic dermatitis (eczema), nasal polyps, asthma and COPD, and many have been impacted by this coverage change – even those who were stable and responding well to treatment.
This isn't limited to FEP. BCBS Dupixent prior authorization requirements and formulary placement vary by state and plan – what's covered under BCBS Illinois Dupixent policies may differ from BCBS Alabama Dupixent coverage. If you've been denied, check your specific plan's formulary and denial reason before assuming another BCBS member's experience applies to you.
When the plan is this strict, your appeal packet needs to be especially tight: an active denial, a clear formulary exception request using the right language, a strong Letter of Medical Necessity, documented failure history, and – if you're stable on the drug – a clear argument for why forcing a switch is medically inappropriate. Especially for conditions like EoE, bullous pemphigoid, and prurigo nodularis, for which Dupixent is the only FDA-approved treatment, the argument for getting a formulary exception is clear and powerful.
How Claimable Can Help
If all of this seems like a lot, that's because it is. Insurers intentionally make the process tough to navigate, so you're more likely to just switch when facing a formulary change. But your treatment should be up to you and your doctor – not up to a rebate deal your insurer made.
We're here to help. Claimable builds customized, evidence-backed appeal letters that combine your personal health story with clinical research, policy analysis, and legal leverage – the three pillars that make appeals successful. This isn't a template or a generic form letter – every appeal is built specifically for your situation, your medication, and your insurer.
Claimable is free for many medications and situations, and otherwise costs just $39.95 + shipping. It's a fraction of the cost of a lawyer, and most cases resolve in under 10 days. We're here to help you navigate next steps. If you've hit a wall with a formulary denial, start your appeal here.
Frequently Asked Questions
Can insurance change my formulary mid-year?
Yes. While most formulary changes happen at the start of a new plan year, insurers can make changes mid-year – including removing drugs or moving them to higher tiers. These can happen at any time but are most common on 1/1 and 7/1. They're required to notify affected patients (typically 60 days in advance), but the notification process isn't always reliable. If you suspect a mid-year change, check your plan's current formulary directly on their website.
Can insurance change my formulary without notification?
They're required to notify you if you're currently on the affected medication. However, if you recently switched plans, changed your coverage level, or are newly prescribed the drug, you likely won't receive advance notice. The notification requirement only applies to patients the insurer already knows are filling that medication.
What is a formulary exception form?
Many formulary exception forms are designed for provider submissions – not patients. If you can't find a patient-specific form (which is common), you can submit a written appeal letter with the required information to your plan's appeals department. Plans are required to accept written appeals even without a standardized form. You can also use Claimable to generate and submit your request.
What is the difference between a formulary exception and a prior authorization?
A prior authorization (PA) is a coverage review required before certain medications will be approved — even if they're on the formulary. A formulary exception asks the plan to cover a drug that isn't on its approved drug list (or to override standard formulary rules). Depending on your situation, you may need to go through one or both processes — and they often happen in sequence, which is why they're easy to confuse.
How long does a formulary exception review take?
Federal rules generally require expedited review within 72 hours for urgent requests and standard review within about 15 days for pre-service appeals — often faster than the typical 30-day window for standard post-service appeals. However, timelines vary by plan type, so always confirm your plan's specific rules and explicitly request expedited review if your situation is urgent.
What if my provider says there's nothing they can do?
This is one of the most common – and most incorrect – things patients hear. Your provider may not be familiar with the formulary exception process or may assume that "not covered" means "not appealable." It doesn't. You have legal rights to challenge formulary decisions regardless of what your provider tells you. Consider sharing resources about the exception process with your provider, or explore your appeal options independently.
Do I need a lawyer to appeal a formulary exception denial?
No. While lawyers can help with complex cases, most formulary exception appeals can be handled effectively without one. What you need is the right evidence, the right language, and knowledge of your rights. Tools like Claimable are specifically designed to help patients build strong, evidence-backed appeals without the cost of legal representation.
Some insurance plans do cover Zepbound for sleep apnea, but coverage almost always requires prior authorization and the right documentation from your provider. If your plan denies the request, that denial is worth appealing, especially since Zepbound is the only GLP-1 medication with FDA approval specifically for obstructive sleep apnea.
The coverage landscape is shifting fast. CVS Caremark dropped Zepbound from its formulary entirely in mid-2025. Multiple class-action lawsuits have been filed challenging these denials. And Medicare now has a specific pathway for Zepbound coverage when prescribed for obstructive sleep apnea (OSA), with a government agreement expected to cap the copay cost at roughly $50/month starting in 2026.
Whether you're trying to figure out if your plan will cover Zepbound before you fill the prescription at your pharmacy, or you've already been denied and need to know what to do next, this guide walks through coverage requirements by plan type, the most common denial reasons, and exactly how to build an appeal that addresses each one.
Does Insurance Cover Zepbound for Sleep Apnea?
Sometimes, yes, but it's usually not automatic.
Coverage generally depends on whether Zepbound is on your plan's formulary, whether you meet your plan's prior authorization requirements, and whether the correct documentation is submitted with the initial request.
Here's why the OSA indication matters so much: Zepbound (tirzepatide) is a GIP/GLP-1 polypeptide receptor agonist and the only GLP-1 medicine FDA-approved to treat moderate-to-severe obstructive sleep apnea in adults with obesity. That means even if your plan limits coverage of GLP-1s for weight loss, you may still have a path to get Zepbound covered for sleep apnea. This distinction is the foundation of most successful appeals.
What Insurers Typically Require for Coverage
This varies by plan, but the most common things insurance wants to see are below. Call your insurer or visit your member website for a full list of coverage criteria. You can see example coverage criteria from CVS Caremark here.
The CVS Caremark Situation
CVS Caremark removed Zepbound from most formularies effective July 1, 2025, after striking a rebate deal with Wegovy's manufacturer Novo Nordisk. Patients have been directed to switch to Wegovy instead.
For OSA patients, this creates a particularly strong basis for a formulary exception: Wegovy is not FDA-approved for sleep apnea. Zepbound is the only GLP-1 with that indication, so there is no formulary alternative with the same FDA-approved use.
As plans renew for 2026, many patients are receiving similar notifications that Zepbound will not be covered in the new year.
Multiple ERISA class-action lawsuits have been filed challenging CVS Caremark's denials.
Medicare Coverage for Zepbound and Sleep Apnea
Medicare Part D may cover Zepbound when prescribed specifically for moderate-to-severe OSA in adults with obesity. This is because Medicare does not cover Zepbound for weight loss alone (federal law excludes anti-obesity medications from Part D unless they have another FDA-approved indication). The December 2024 OSA approval created the coverage pathway that didn't exist before.
CMS proposed expanding Part D to include anti-obesity medications for 2026, but the government decided against it, which means the OSA indication remains the only Medicare pathway for Zepbound.
Key details for Medicare plans:
- Coverage depends on whether your specific Part D plan has added Zepbound for OSA to its formulary. Check using the Medicare.gov Plan Finder or call the number on your card.
- Starting as early as April 2026, a government agreement with Eli Lilly is expected to cap the Medicare copay at approximately $50/month.
- The 2026 annual out-of-pocket costs for Part D is $2,100.
- Medicare Advantage plans (Part C) vary; some have added Zepbound for OSA, others haven't.
- Prior authorization is almost always required.
- Lilly savings cards are not available to government-insured patients (Medicare, Medicaid, Tricare).
If your Part D plan denies coverage, Medicare has its own escalation path: redetermination within 120 days, then QIC reconsideration, then ALJ hearing.
Common Denial Reasons and What to Do About Each One
When it comes to Zepbound for sleep apnea, all of the common denial reasons can be challenged. It's about identifying the right steps to take. Look for language like these in your denial letter under "why your request was denied."
Need help figuring out which reason applies to you and what strategy to use? Use Claimable's guided appeals tool to make it easy.
Prior Authorization Incomplete / Missing Documentation
What it looks like: "Insufficient information," "missing documentation," "clinical records not provided."
What to do: Contact your prescriber's office to find out exactly what was submitted. Compare it against your plan's requirements, then resubmit with a complete packet: sleep study, BMI documentation, diagnosis notes, and treatment plan.
"Not Medically Necessary"
What it looks like: "Does not meet criteria," "not medically necessary."
What to do: Get a copy of your plan's coverage criteria and compare it against your records point by point. File an appeal that directly addresses each criterion, and include a letter of medical necessity from your healthcare provider. If your insurer's criteria don't align with FDA labeling or clinical guidelines, flag that in the appeal.
Not on Formulary
What it looks like: "Not covered," "non-formulary," "preferred alternatives required."
What to do: Appeal and request a formulary exception. Since Zepbound is the only GLP-1 approved for sleep apnea, your exception request has a strong foundation. If the plan is suggesting Wegovy or another GLP-1, those drugs are not FDA-approved for OSA. Clearly state why the suggested alternatives are not appropriate for your diagnosis.
Plan Exclusion / "Weight Loss Only"
What it looks like: "Plan excludes weight-loss medications," "not a covered benefit."
What to do: This is a mis-categorization issue. Zepbound prescribed for OSA is a treatment for a sleep disorder, not a weight-loss prescription. Confirm with your provider that the PA was submitted under ICD-10 code G47.33 (OSA), not obesity. If the coding was correct and the denial still cites a weight-loss exclusion, appeal and clearly distinguish between the two indications.
Step Therapy / Alternative Required
What it looks like: "Must try X first," "step edit."
What to do: If you've already tried alternatives (CPAP, other medications, lifestyle interventions) and they didn't adequately manage your OSA, document those attempts in your appeal. Note that no other GLP-1 is FDA-approved for OSA. Also, 37+ states have step therapy protection laws that may limit your insurer's ability to enforce these requirements.
How to Appeal a Zepbound Sleep Apnea Denial
Most people will be able to reverse a Zepbound denial for sleep apnea when they appeal with the right argument, documentation, and clinical backing. Here's the high-level process.
Your appeal should mirror the denial reason. Quote the denial reason directly, respond with the specific evidence that addresses it, and attach supporting documents with the relevant sections highlighted. Key documents include your denial letter, sleep study report, OSA diagnosis/severity, BMI documentation, provider notes, and (recommended) a letter of medical necessity from your prescribing provider.
Important deadline: Most commercial plans give you 180 days from the denial date to submit an internal appeal. Don't miss it.
If your first appeal is denied, you can request a second-level internal appeal. After exhausting internal appeals, most plans are required by law to offer access to external review through an independent organization. Your final denial letter should include instructions on how to request it.
Read our full guide to appealing a Zepbound denial for a detailed, step-by-step walkthrough of the appeals process.
How to Get Ahead of a Denial Before It Happens
If your doctor is considering prescribing Zepbound for sleep apnea, you can get ahead of coverage issues from the start.
What to ask your insurer (call the number on your insurance card):
- Is Zepbound covered for obstructive sleep apnea under my specific plan?
- Is it on formulary? If not, what's the exception process?
- What are the prior authorization criteria, and where is the PA form?
- Where should the PA be submitted (portal/fax)?
- What are typical timelines, and what qualifies for an expedited review?
What to confirm with your provider before the PA is submitted:
- Sleep study report and AHI documentation are attached
- Current BMI/weight documentation is included
- Diagnosis is coded under OSA (G47.33), not obesity
- Clinical rationale ties directly to the plan's stated criteria
- Submission goes to the correct portal or fax number
Ongoing Legal Challenges to Zepbound OSA Denials
Several lawsuits are now challenging insurers' categorical denials of Zepbound for sleep apnea. A class-action suit filed in September 2025 alleges CVS Caremark and CareFirst BlueCross BlueShield wrongfully denied coverage in violation of ERISA. A separate suit in New York challenges CVS Caremark's blanket formulary removal. And a third targets Elevance (Anthem) for denying OSA coverage while covering other GLP-1s for different conditions.
These cases are still in progress, but they signal that many denials may not be consistent with plan terms or federal law. Learn more about the legal landscape here.
How Claimable Helps
Navigating insurance appeals is time-consuming and confusing, especially when you're dealing with a condition that affects your sleep and daily functioning. Claimable's appeals tool helps you:
- Identify the most likely reason behind your denial
- Build a customized appeal letter backed by clinical evidence, policy analysis, and relevant legal protections
- Automatically mail and fax your appeal to the right place
- Escalate to the next level if your first appeal is denied
Start your Zepbound sleep apnea appeal with Claimable →
FAQs
Does insurance cover Zepbound for sleep apnea? Some plans do, but coverage typically requires prior authorization. Your provider will need to submit documentation including your sleep study, OSA diagnosis, and BMI. If your plan denies coverage, you have the right to appeal.
What do I do if insurance denies Zepbound for sleep apnea? Get your denial letter and identify the specific reason. Common reasons include missing documentation, "not medically necessary," formulary exclusion, benefit exclusion, or step therapy requirements. File an appeal that directly addresses the stated denial reason with supporting evidence.
Does Medicare cover Zepbound for sleep apnea? Medicare Part D may cover Zepbound when prescribed for moderate-to-severe OSA in adults with obesity. Medicare does not cover it for weight loss alone. A government agreement is expected to cap the Medicare copay at approximately $50/month starting as early as April 2026.
Does CVS Caremark cover Zepbound? As of July 2025, CVS Caremark removed Zepbound from its standard formulary. However, since Zepbound is the only GLP-1 FDA-approved for OSA, you may have strong grounds for a formulary exception.
Can I appeal a plan exclusion denial for Zepbound for sleep apnea? In many cases, yes. Most benefit exclusions apply to weight-loss medications. Since Zepbound is FDA-approved for OSA, a prescription for sleep apnea should not fall under a weight-loss exclusion. Appeal and clearly distinguish between the OSA and weight-loss indications.
What is a formulary exception? A formulary exception is a request for coverage of a medication that isn't on your plan's list of covered drugs. For Zepbound and OSA, the exception argument is particularly strong since no other GLP-1 has FDA approval for sleep apnea.
How long do I have to file an appeal? Most commercial plans give you 180 days. Medicare patients have 120 days. Check your denial letter for exact deadlines.
What clinical evidence supports Zepbound for sleep apnea? The SURMOUNT-OSA trials showed Zepbound reduced breathing disruptions by 55-63% over 52 weeks. Up to 51.5% of participants no longer met OSA criteria after one year.
Let's get you covered.


